28th December
2022
First of all, in rural India visiting a government health facility when one needs to consult a health practitioner is not at ubiquitous as one would assume. A survey, carried out by the Development Intelligence Unit (promoted by Transforming Rural India Foundation and Sambodhi Research and Communications), reveals that only in 57% of the cases has this been the preferred treatment seeking behaviour. This is in line with NFHS 5 which had estimated that 49.9% of rural India do not generally use a government health facility
Consumer satisfaction with accessing health services in rural India
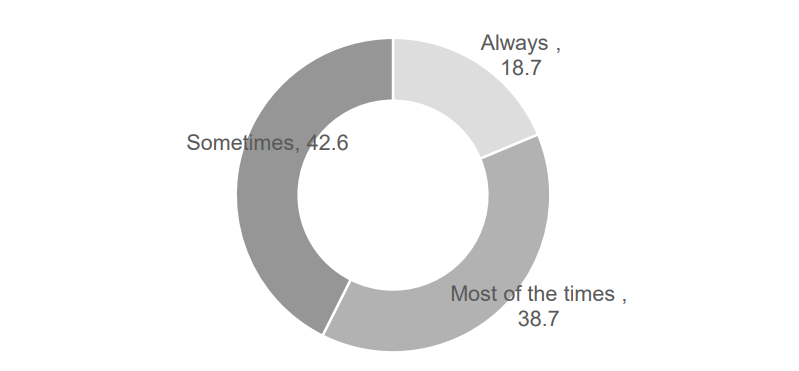
How often do you use government health facilities when you need to see a health practitioner? [Figures in percentage]
Nevertheless, Sub Centres, PHCs, CHCs, Civil/District Hospitals and Teaching Hospitals remain important sources of healthcare for the rural masses with a typical rural household having at least one member having visited a government facility at least once in the past 3 months.
However, what is surprising is that visit to a PHC or higher order facility was reported to be much more than visited a health sub centre, which is designed for last mile connectivity.
What type of health facility did you visit?
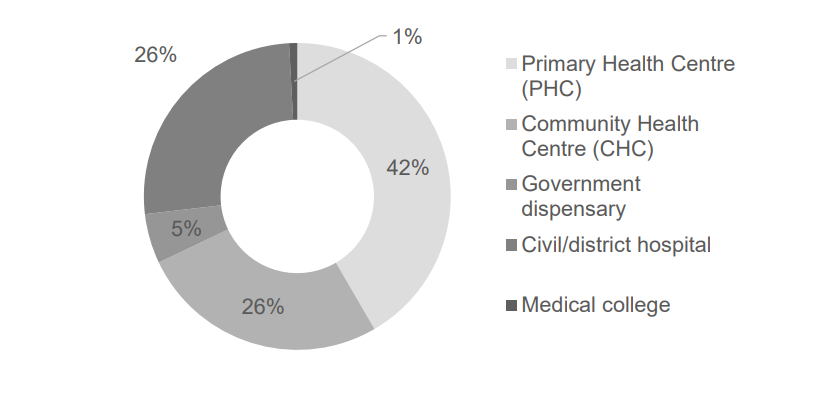

As per the rural survey, only 8.5% of the rural respondents had gone to a sub centre during their last visit to a government health facility. The preference seems to be clearly towards a higher order facility, preferably where a qualified doctor is also available.
Based on available literature on the subject, perhaps one of the reasons behind the sub-optimal utilization of sub centres could be the fact that many ANMs prefer not to stay alone in their allotted sub centres because in most cases, sub centres are built on land 2-3 kms from the nearest habitation as it is mandated that they have to be constructed on free plots as they are ‘social infrastructure’. Secondly, ANMs duties require them to be quite mobile, going from one village to another within their catchment attending VHNDs and administering routing immunization and counseling to pregnant and lactating mothers.
However, it may be worth mentioning that they survey data indicates to the contrary with 83% of those who had visited a sub centre during their last visit to a government health facility did report that they had met the ANM. 12.4% were serviced by the Male Health Worker (MPW-M). In fact, just around 3% had reported that no-one had attended to them at the sub centre during their last visit.
For all other higher order facility, 92.5% could manage to consult with the resident doctor during their last visit.
Given that health delivery through the government system is free of charge, an inquiry was made as to whether or not respondents were faced with a demand for bribe, be it for consultation, tests, or medicines. 97% of the survey participants had reported that they had not been approached for a bribe and a mere 1% had actually done so.
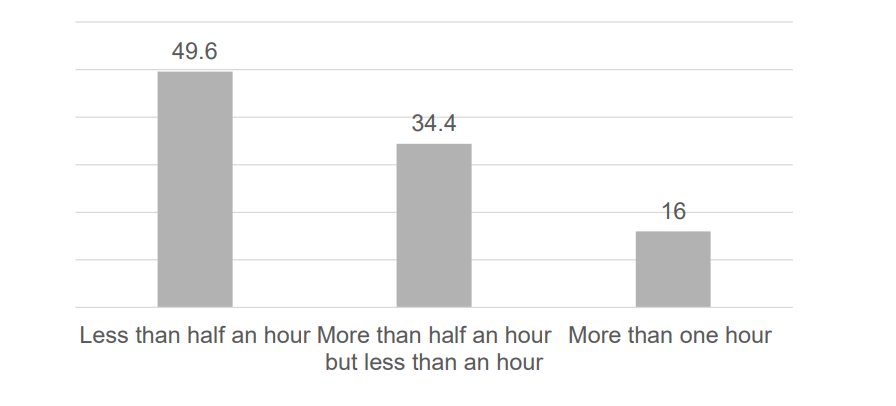
For nearly half of the respondents, the waiting time to see a health service provider (doctor or ANM) was less than half an hour; for 94%, it was less than an hour.
If you saw a doctor or an ANM, then how long did you have to wait to see him/her during your last visit? [Figures in percentage]
Nearly 70% of the respondents could confirm that the health provider whom the consulted was not rude and was attentive and interested in carrying out the investigation into their health issue. 87% thought that their examination seems to have been thorough.
However, and at the same time, perceived rudeness in behaviour (of varying degree) was also reported, by 28.7% of the respondents.
Despite this, the positive feedback was that just over 91% of the respondents had felt that the healthcare professional who was consulted was attentive and at least gave off appositive vibe (interested) while attending to them.
Were you given a prescription and free medicines? [Figures in percentage]
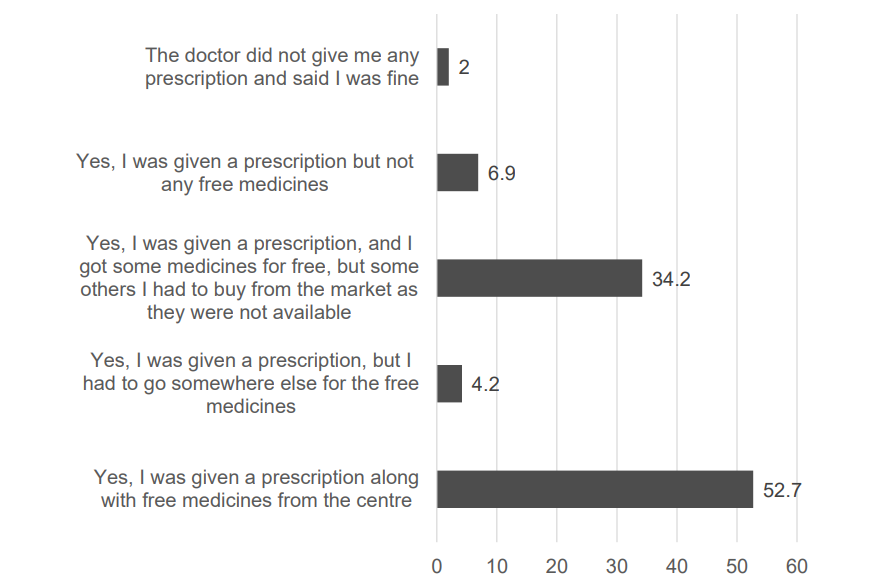
The survey revealed that close to 53% of the respondents could confirm that they were given a prescription along with free medicines from the centre. At the same time, had to buy all or some of the medicines through the open market as they were not available at the centre. This finding is fairly similar to the estimation brought out by the Economic Survey 2019-20 which observes that 60% of the patients are still forced to pay for some of the medicines that are being prescribed by government health facilities.
This survey was conducted among 4547 individuals who had visited a government health facility at least once over the past 2 years, either for their own treatment, or had accompanied someone who required treatment. The survey covered a total of 20 states and the entire sample was from rural India. The survey was run by SambodhiPanels. The survey was run in August 2022